Head trauma in veterinary medicine
Lisa Lipitz, VMD, DACVIM (Neurology)
Neurology/Neurosurgery, Bush Veterinary Neurology Service, Rockville, MD
Posted on 2018-12-11 in Neurology
Today’s post was originally published in Neurotransmitter, Bush Veterinary Neurology Service’s online newsletter. Modified and reprinted with permission.
Traumatic brain injury in dogs and cats can occur due to a variety of causes including motor vehicle accidents, falls from a height, crush injuries, or attacks by other animals. This event secondary to a serious accident can be terrifying for owners and is a veterinary emergency for the injured patient. Initial patient assessment and rapid initiation of appropriate treatment measures are critical to maximize the chance for a successful outcome. Appropriate guidelines for veterinary patients are somewhat limited and, therefore, often based on results of human trauma studies, experimental investigations, and clinical experience.
Patient Assessment
Modified Glasgow Coma Scale (MGCS)
One quantitative measure shown to be associated with survival in dogs with traumatic brain injury is the Modified Glasgow Coma Scale. This scale has been shown to predict the probability of survival in the first 48 hours in patients with traumatic brain injury.1It is therefore most useful for initial patient assessment; however, it can also be used as an objective way to monitor progression of neurological signs on a serial monitoring basis. The MGCS provides a score that addresses the three domains listed below. A score of 1-6 is assigned to each category; the final score ranges from 3 – 18, with lower scores indicating more severe neurologic deficits.
1. Level of consciousness
- Alert and responsive: normal responses to sensory stimuli
- Obtunded: slow/inappropriate responses to sensory stimuli
- Stuporous: unresponsive except to noxious stimuli
- Comatose: completely unresponsive to repeated noxious stimulation
- Pupil response to light and other brainstem reflexes (palpebral, corneal, gag)
2. Pupil response to light and other brainstem reflexes (palpebral, corneal, gag)

Modified from de Lahunta and Glass. Veterinary Neuroanatomy and Clinical Neurology, 3rd ed. St. Louis, MO: Elsevier Inc; 2009.
3. Posture and motor activity (1-6)
- Ambulatory vs. non-ambulatory status
- Abnormal postures
- Decerebrate rigidity = stupor/coma, rigid extension of all 4 limbs, opisthotonus (brainstem lesion)
- Decerebellate rigidity = conscious/mentally alert, rigid extension of thoracic limbs, flexion of pelvic limbs, opisthotonus (cerebellar lesion)
In 38 dogs with head trauma, the MGCS predicted the probability of survival in the first 48 hours. The graph below illustrates there is a 50% probability of survival in a patient with a score of 8; patients with scores higher than 8 have a higher probability of survival compared to patients with lower scores.2
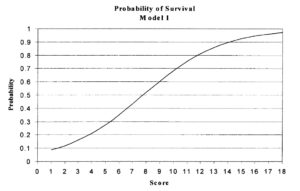
From Platt SR, Radaelli ST, McDonnell JJ. The Prognostic Value of the Modified Glasgow Coma Scale in Head Trauma in Dogs. J Vet Intern Med 2001; 15:581-4.
Diagnostics
Complete bloodwork (an initial PCV/TS, blood glucose, and electrolytes followed by a complete cbc/chemistry panel) as well as assessment of the abdomen and chest for signs of trauma (if indicated) should be obtained. Radiographs of the head can be taken to screen for the presence of skull fractures. Imaging of the brain in head trauma patients is via CT or MRI examination; these advanced imaging tests provide assessment of both skull and brain damage. In a recent study of 18 dogs with acute head trauma, dogs with parenchymal brain injuries affecting the caudal fossa (brainstem/cerebellum) alone or affecting both the rostral (forebrain) and cauda fossa typically had poorer outcomes.3 If a patient’s neurological status continues to decline despite aggressive medical treatment, then evaluation of the extent of brain damage via CT or MRI exam and consultation with a veterinary neurologist is indicated.
Therapy
The goals of treatment in traumatic brain injury include reducing intracranial pressure, maintaining blood pressure, and ensuring proper ventilation. Hyperosmolar therapy reduces brain edema. Mannitol is a hyperosmolar osmotic diuretic which is considered the first line treatment for reducing intracranial pressure; administration of mannitol (0.5-2 grams/kg as an IV bolus over 20minutes q6-8 hours) has been shown to have a beneficial effect on neurological outcome in human and veterinary patients with brain injury. Hypertonic saline (3-5ml/kg) is another hyperosmolar solution with effects similar to mannitol which can be used to reduce intracranial pressure and rapidly provide intravascular volume expansion. Other important steps in managing trauma patients include intravenous fluid therapy to prevent hypotension, placing patients in an oxygen-rich environment to prevent hypoxia, and close monitoring of ventilation to prevent hypercarbia. Analgesic care should be given as needed with opioids or other reversible medications. If there is a risk for infection, antibiotic therapy should be provided to reduce the risk of an abscess from developing. Importantly, glucocorticoids are contra-indicated and should not be given to patients with brain injury; administration of steroids is associated with worse outcomes in human adults with head trauma. A helpful clinical practice review article from the Journal of Veterinary Emergency and Critical detailing medical management recommendations for patients with traumatic brain in is provided below in the article references.4
In the event that medical therapy is unsuccessful, surgical treatment (decompressive craniectomy) may be necessary for patient stabilization. This is the case with depressed skull fractures, large space occupying hematomas, or intracranial abscessation.
Prognosis
There is scarce available information that is predictive of prognosis in veterinary medicine for patients with traumatic brain injury. However, many patients can recover if systemic and neurological abnormalities are identified and treated early. Dogs and cats have an extraordinary ability to compensate and improve after sustaining brain damage. Longterm effects such as post-traumatic epilepsy are reported to occur in a small percentage of patients with head trauma; in one retrospective study of dogs with epilepsy, 15% of dogs had a history of prior head injury.5 Ultimately, patient response and degree of improvement to treatment over time ultimately determines the prognostic outcome.
References
- de Lahunta and Glass. Veterinary Neuroanatomy and Clinical Neurology, 3rd ed. St. Louis, MO: Elsevier Inc;2009.
- Platt SR, Radaelli ST, McDonnell JJ. The Prognostic Value of the Modified Glasgow Coma Scale in Head Trauma in Dogs. J Vet Intern Med 2001; 15:581-584.
- Yanai H, et al. Results of magnetic resonance imaging performed within 48 hours after head trauma in dogs and association with outcome: 18 cases (2007-2012). J Vet Am Med Assoc 2015;11(1):1222-1229.
- Sande A and West C. Traumatic brain injury: A review of pathophysiology and management. Journal of Vet Emerg and Crit Care 2010;20(2):177-190.Steinmetz S, et al. Epilepsy after head injury in dogs: a natural model of posttraumatic epilepsy. Epilepsia 2013; 54(4):580-8.
About the author
Prior to relocating to the Maryland/DC area, Dr. Lipitz worked as a staff Neurologist at a specialty and emergency hospital in Coral Springs, Florida. Dr. Lipitz enjoys lecturing and has given continuing education seminars to veterinarians as well as presented her research at the ACVIM conference. She has several publications to her credit in the areas of infectious brain disease, neoplastic brain disease, and congenital spinal disorders. Outside of work, Dr. Lipitz enjoys spending time with her husband Chad, their son Chase and daughter Cate, and lovable Labrador, Keyes. |


 Dr. Lipitz, a New Jersey native, received her undergraduate and Doctorate of Veterinary Medicine degrees from the University of Pennsylvania. She completed a small animal rotating internship at Tufts University in 2005. Following this academic training, Dr. Lipitz worked in private practice for three years as an emergency and critical care veterinarian at the Veterinary Specialty and Emergency Center in Langhorne, Pennsylvania. In 2008, Dr. Lipitz went on to complete her Neurology and Neurosurgery residency at the University of Wisconsin-Madison; she received her ACVIM Board Certification in June of 2011. Dr. Lipitz completed additional continuing education and earned her ACVIM Certificate of Neurosurgery Training in May of 2012.
Dr. Lipitz, a New Jersey native, received her undergraduate and Doctorate of Veterinary Medicine degrees from the University of Pennsylvania. She completed a small animal rotating internship at Tufts University in 2005. Following this academic training, Dr. Lipitz worked in private practice for three years as an emergency and critical care veterinarian at the Veterinary Specialty and Emergency Center in Langhorne, Pennsylvania. In 2008, Dr. Lipitz went on to complete her Neurology and Neurosurgery residency at the University of Wisconsin-Madison; she received her ACVIM Board Certification in June of 2011. Dr. Lipitz completed additional continuing education and earned her ACVIM Certificate of Neurosurgery Training in May of 2012.