My dog hasn’t pooped since discharge! (5 min ago)
Why clients don’t remember what we tell them
Mark Troxel, DVM, DACVIM (Neurology)
Massachusetts Veterinary Referral Hospital, Woburn, MA
Posted on 2016-09-27
Studies in human medicine over the past 30-40 years have shown consistent poor recall of medical information, with between 40-80% of all medical information being immediately forgotten. In fact, 48% of information that is “remembered” is either imagined or misconstrued. As veterinary medicine becomes increasingly complex, it is critical that our clients are able to successfully recall the medical information that we provide to ensure the health and well-being of our patients. To this author’s knowledge, there are no studies in veterinary medicine examining medical information recall. However, in human medicine, studies examining medical information recall have been conducted since the 1960s. This article provides an overview of medical information recall studies in human medicine.
The terminology used to describe recall of medical information has changed over the past few decades. A frequent statement made by physicians and veterinarians is that our owners are “not compliant.” Compliance is a term that implies that the patient does what the doctor orders. There is little to no patient involvement in the decision-making process. This term is used less frequently these days because it implies a paternalistic relationship. Nowadays, compliance has been replaced by the term adherence because it implies that there is active patient involvement in the decision making process, which theoretically translates to better patient recall of information and persistence, a term meaning that the patient follows the directions long-term.
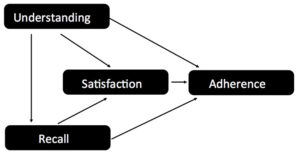
Adherence is related to patient understanding, ability to recall medical information, and satisfaction with the doctor, as shown below in Stephen Ley’s model of patient factors vs. adherence.
 |
Forgetting medical information falls into 3 categories
- Factors related to the doctor
- Factors related to the patient
- Method of delivery
Factors related to the doctor
There is a 3-step process in any interaction between the clinician and patient/owner, (1) creating a good interpersonal relationship, (2) exchange of information, and (3) medical decision-making. The educational theory that most people understand is pedagogy, in which learning is teacher driven, and was the cornerstone of medical education until recently. The teacher (clinician in our case) determines the nature and scope of the educational program for a passive and cooperative learner. Many medical educators now recommend andragogy, an adult learning theory described by Malcolm Knowles that has been shown to increase adherence in adult patients. In this model of learning, the teacher’s role is one of mutual participation with the learner where the teacher (clinician) facilitates, promotes, and encourages active involvement by the learner (patient/client).
Diane McCann, EdD and John Blossom, MD looked at 28 studies investigating the physician-patient relationship and found 5 basic steps in the educational process that parallel the sequence of activities in the physician-patient relationship.
- Establishing a rapport with the client
- Assessing the patient’s needs
- Developing a plan
- Implementing the plan
- Evaluating the plan
Clinicians can’t do every step at every meeting due to time constraints. Rather, specific behaviors vary from time to time depending on the circumstances. The following guidelines were developed around the mnemonic, ADULT.
A Establish a rapport by eliciting the patient’s ACTIVE involvement
D Assess the patient’s needs by carefully listening as the patient DISCUSSES their concerns
U Develop a plan by promoting an UNDERSTANDING of the issues
L Implement a plan by offering the patient opportunities to LEARN new behaviors
T Evaluate the plan by identifying strategies for TRACKING the patient’s progress
Establishing a rapport 
Numerous studies have examined the important of establishing a rapport with the patient. Perhaps most directly related to veterinary-client relationships, studies of parents of children seen at an emergency clinic were more likely to follow medical advice when the physician was courteous, friendly, and personable. The greater the degree of friendliness, the more likely the parent was to follow the medical advice. Additionally, increased adherence occurs with patient-centered interviews, those in which the patient has the freedom to freely provide historical information rather than just being driven by the clinician.
Assessing the patient’s needs
Korsch et al. studied 800 acutely ill children brought to an ER Department. Of 625 parents who said their physician understood their concerns, 83% expressed satisfaction and adhered to the plan. Of the 80 parents that thought the physician didn’t understand their needs, only 32% expressed satisfaction and were cooperative.
Linn and Wilson studied patient interaction skills of 76 interns/residents. They found a lower “no show” rate on patient rechecks for physicians trained to explore the patient’s thoughts/feelings in a non-authoritarian manner. Additionally, personal telephone cancellation, rather than simply not showing up, was higher in these trained physicians, potentially suggesting the patient was more likely to continue following the previous medical advice and follow-up at a later date.
Develop a plan
Adherence is higher when the physician develops a plan in conduction with the patient. For example, Starfield, et al. examined the importance of patients concerns as an essential step in the process of medical care. They found increased follow-up adherence when both the patient and clinician agreed on the necessity of follow-up care. Increased patient participation was also associated with overall health improvement. Health improved for 63% of the problems recognized by both the patient and clinicians as being important compared to only 22% for problems thought important by the patient only. Increased parent adherence has been documented when the physician provided feedback by explaining the diagnosis and its cause.
Implement the plan
Increased adherence has been found when there is a multimodal process for implementing the health plan. The first step is individualized instruction (one-on-one instruction between a healthcare worker and the patient) where the patient is provided sufficient time express their concerns/needs and to learn about their condition and its treatment. Adjunctive instruction between the patient and other health professionals (e.g., nurses) under the supervision of the patient’s physician further improves adherence. Haynes, et al studied 38 hypertensive Canadian steelworkers that had not met blood pressure (BP) goals or adhered to prescribed program in past 6 months. Patients in the experimental groups were taught to take their own BP, chart their BP and pill taking. They were taught to adjust pill taking to their daily habits and rituals. They were then monitored biweekly and praised for adherence and when their BP was noted in a log. Six months later, the adherence in the experimental group had risen by 21.3% while control group fell by 1.5%. The BP fell in 85% of experimental patients compared to 55% of control patients. Finally, referral to an educational program, such as a diabetes educational clinic, increases patient adherence and persistence.
Evaluating the plan
Several factors have been identified with regard to increasing adherence. These include providing the opportunity for patients to ask questions, evaluating the patient’s understanding of the plan, working with patients to overcome obstacles to adherence (e.g., the difficulty for a veterinary client giving a TID medication compared to a BID medication), giving encouragement, support, and reassurance, monitoring the patient’s progress, and recording the plan in the medical record so that everyone is on the same page with the plan.
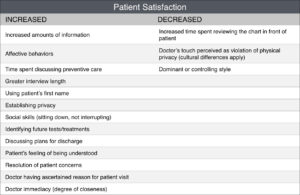
Specific doctor communication behaviors
Several broad categories of doctor communication behaviors have been investigated:
Instrumental vs. affective
Instrumental (or task-focused) behaviors include giving information, asking questions, counseling, giving directions, identifying future treatment or tests, discussing side effects, discussing test results, etc. We’re all good at instrumental behaviors, but less so with affective (socioemotional) behaviors including things such as being “very encouraging, relaxed, friendly, open, and honest.” One could argue that veterinarians are more likely to show affective behaviors than our physician counterparts. Interestingly, human oncologists sometimes deliberately withhold information. One study found that < 40% of oncologists actually used the word “cancer” in fear that it will cause strong negative emotional reactions. Studies are conflicting as to whether patients can distinguish instrumental vs. affective behaviors from their doctors, but it certainly plays a role in their view of the physician and, in turn, how much they remember.
Verbal vs. non-verbal behavior
Non-verbal behavior includes tone of voice, gaze, posture, laughter, facial expressions, touch, and physical distance. Only 7% of emotional communication is conveyed verbally – 38% is by tone of voice and 55% is by visual cues (eye contact, body position, etc.). For example, women with breast cancer remembered less if their doctor looked worried.
Privacy behaviors
This is a bit less of a concern in veterinary medicine, but we still have to deal with privacy issues. In human medicine, there are three types of privacy: psychological, social, and physical privacy. Psychological privacy is centered on the patient’s willingness to share personal and revealing information. Social privacy relates to the patient’s ability to manage interactions or maintain status divisions – in other words, the degree of formality in a situation and how personal the conversational topics and language are. For example, sustained eye contact may be perceived by the patient as too intimate. Physical privacy relates to the patient’s personal space. In human medicine, this is a huge topic, less so in our field, but studies have shown that some (many?) patients don’t want to be touched outside what is literally required.
High vs. low controlling behaviors
These behaviors relate to who has the most “control” in the interaction, the doctor or patient. Traditionally, medical interactions tend to have high physician control, which is a more paternalistic behavior. There is a move toward a better balance between doctor-centered and patient-centered interactions.
Medical vs. everyday language
Doctors must communicate both in medical language and their everyday language. The ability to communicate in everyday language for a non-medical clientele is critical to increasing patient satisfaction, understanding, and adherence. A study by Bourhis, et al. found that physicians reported switching from medical language (ML) to everyday language (EL), but patients and nurses did not perceive this shift. The reverse is also true. Patients reported attempting to switch to ML, but doctors did not register that a change had occurred.
 |
Factors related to the patient (client)
Age-related memory
Prior to discussing age-related memory, a brief description of the types of memory is in order. Procedural memory is unconscious, unintentional recall of how to do things, such as swimming or riding a bike, while declarative memory is conscious recall of factual information such as dates, words, faces, events, and concepts. Declarative memory is further divided into semantic & episodic memory. Semantic memory, the recall of general facts, such as remembering the rules of soccer or that Washington, DC is the capital of the US, is relatively spared as people get older. However, episodic memory, the recall of personal or individual facts, in this case what the doctor tells you, IS subject to age-related memory decline.
Some have speculated that age-related recall problems are due to difficulty encoding & storing information rather than ability to retrieve information. Studies have shown a moderate inverse relationship between age and amount of information recalled correctly. Additionally, studies have shown that older adults have more difficulty structuring information to be stored in memory. This was demonstrated by McGuire in a prospective study by that examined retention rates in young adults vs. older adults. The younger adults were all college students in a psychology class at 1 of 3 local private colleges and the older adults were recruited from newsletters and announcements at 6 local senior centers. They were shown a video designed to simulate a consultation at a physician’s office. The video was recorded in either an organized or unorganized manner – both videos had the exact same information. Organized material presented was presented in the following order: test results, diagnosis, treatment, prognosis and miscellaneous. An unorganized manner of presentation was also tested, which is probably more real world because either information flows in over time or patients/owners frequently interrupt doctor to ask questions that throws the doctor’s script off track. Medical information retention was tested immediately, at one week, and at one month. McGuire found that only 22% of information was correctly recalled immediately overall by both groups, which subsequently dropped to 17% at one week and 13% at one month. There was a significant difference in age groups immediately after presentation of the medical information. The young adults were significantly better able to correctly recall information than older adults immediately after presentation but, at one week and one month there was no significant difference between younger and older adults.
Another study by Jansen, et al. examined 260 newly referred Study by Jansen et al looked at information recall in 260 newly referred cancer patients. The patients completed a questionnaire to assess information needs and anxiety. Recall was then measured by structured telephone interview within 10 days of discharge compared to audiotapes recorded during the consultation. They found that recall decreased significantly with age, but only when the total amount of information was taken into account. In general, recall was less for the following categories: older patients, poor prognosis, and increased information presented regarding prognosis.
Retention vs. prior knowledge/beliefs
Several studies have examined the extent to which information is recalled compared to prior knowledge or beliefs. They found that medical information is better remembered if the medical information is new or confirms preexisting knowledge or beliefs. This is explicable in terms of cognitive schemas, a term used in psychology. A schema is a “personal theory” formed by an individual over the years about a disease or disorder, but frequently contains inaccuracies or misconceptions. New information inconsistent with the person’s schema tends to be misinterpreted or forgotten. In several studies, “disconfirming” information was recalled less accurately than “confirming’ information. Recall was worse when medical information was related to the patient’s own illness and had personal relevance. Additionally, it was easier to process/store/recall new information than to correct preexisting incorrect knowledge.
 Recall vs. patient anxiety/distress
Recall vs. patient anxiety/distress
There are 2 psychological phenomena related to client/patient anxiety/distress that are relevant in the clinical setting, namely attentional narrowing and state dependency. Attentional narrowing occurs when peripheral information is not processed and stored after the client hears the primary information. In other words, clients do not hear additional information after the primary patient focus of “Your dog has an inoperable brain tumor” has been presented. For example, clients may not remember that their pet will likely continue to have seizures even on anticonvulsants or that prednisone causes PU/PD. State dependency also plays a role in recall. The amount of information recalled also depends on congruity between physical and psychological states at time information presented and when recalled. Memory performance is best when the patient is in the same psychological state, and studies have shown that memory is best when the patient is at a moderate level of anxiety and low when the patient is either at a low or high level of anxiety (i.e., an inverse U-shape).
Predicting forgetfulness
Multiple studies have found a linear relationship between number of statements presented and number of statements that were not recalled. Ley and others did linear regression to derive an equation to predict forgetfulness:
y = 0.56x – 0.94
where x = number of statements made by the doctor and y = number of statements forgotten
This equation predicts the number of statements forgotten +/- 1 in 77% of patients, and predicts exactly in 42% of patients. For example, if the doctor makes 5 statements, the predicted number of forgotten statements will be 1.86.
Influence of health literacy
Health literacy has been linked to comprehension of health-related information. McCarthy et al. examined the recall rate compared to health literacy. In the study, 755 patients, ages 55-74, were shown of hypothetical video of either wound care management (simulating an emergency discharge) or diagnosis and treatment of GERD (simulating a GP diagnosis). Each patient then asked a series of 7 questions related to the discharges. They found 71.6% of the patients had adequate health literacy skills and performed significantly better than those with marginal or low health literacy skills. The higher the health literacy level, the greater the recall, but all groups had decreased recall when retested at a later date. On several questions, such as “When does your doctor want you to take your pill?”, the low and marginal health literacy groups had < 50% recall rate.
Perceived importance of medical information
Several studies have shown amount recall is related to patient’s subjective assessment of importance. In several studies, the diagnosis was perceived as more important and better remembered by patients than the treatments recommended by the doctor.
Method of delivery
How the medical information is delivered has been examined extensively, including method of delivery (e.g. verbal vs. written), serial position of information, repetition, specific vs. general instructions, wording/language, and multimedia presentations.
Method of presentation
One would think that a combination of oral and written instructions would improve medical recall. However, a study by Ley examining primacy and rated importance of medical information found that there was little difference in recall between oral (48.1%), visual (44.2%) and a combination of oral and written instructions (50.4%).
Serial position
The same study by Ley listed immediately above examined recall vs. the serial position in which the information was presented. As expected, the first third of information presented was remembered better (55.5%) than the second third (44.5%) and last third (42.6%) of the information.
Method of delivery
Ley also found that there was improvement in in memory when instructions and advice were given first (87.3%) compared to the usual method of delivery (e.g., test results diagnosis treatment prognosis).
Use of pictographs
Several studies have shown improved medical recall when the discharges included pictographs, simple cartoons and illustrations reflecting the written text, such as a caricature of a doctor in standing at an easel with medical information “written” on the board.
Multimedia presentations
As computer technology has increased markedly over the past few decades, one would think that the ability to create elaborate multimedia presentations with animations and videos would improve recall and adherence. Unfortunately, to date, multimedia discharges and health information have not been found to improve adherence and persistence.
Repetition of information
The effects of repetition of information have not been consistent across multiple studies, which have found that, while there is improvement in immediate recall in patients given repetitious information, this improved recall was no longer present several weeks later.
Specific vs. general statements
In general, people tend to better remember specific statements than general statements. Bradshaw, et al. examined recall of medical advice as it relates to comprehensibility and specificity. They found that specific statements have higher recall rates than general statements. For example, a general statement, such as “You must lose weight” is remembered less often than a specific statement, such as “You must lose 30 pounds.”
Use of after visit summaries
Recent legislation in the USA has made it all but required an “after visit summary” (AVS; i.e., discharge instructions) for all patient encounters in human medicine to be eligible for financial incentives from Medicare/Medicaid. Pavlik, et al. looked at patient recall, satisfaction, and adherence to the content of various forms of AVS. They included 4 types of AVS: (1) minimum, (2) intermediate, (3) maximum, and (4) and their standard clinic AVS. Recall was measured at 2 days and 2-3 weeks after the office visit. Their results showed that most patients liked receiving printed material (70% agreed, 24% strongly agreed). One might assume that providing the patient with a long AVS with a lot of medical information regarding diagnosis, treatment and prognosis would improve patient satisfaction and adherence, but in this study, fewer patients felt the longer AVC presented the “right amount of information,” preferring instead a shorter AVS. When asked to recall the categories of information (e.g., diagnosis, medications, and prognosis), medications (broad category, not individual medications) was the only category remembered by > 50% of the participants. Patients given a shorter AVS had the greatest recall (32%) of categories as a proportion of total numbers of categories. At the beginning of the study, the authors asked the participants about the planned disposition of the AVS after the initial office visit. Less than 30% of patients planned to save the AVS and less than 1% planned to save it for their next primary care visit. What actually happened to the AVS? The authors found that 51% of participants filed the AVS with their health records and only 12.5% of participants read it once. For clients that chose “Other” when asked what they did with the AVS, 44% of them stated they had left it somewhere in their car or somewhere in the house to be filed.
 Conclusion
Conclusion
It is clear that patients/clients will be unable to remember a significant portion of the medical information presented to them, regardless of doctor and patient/client traits and how the medical information is presented. However, there are clearly things that we can do to improve recall:
- Use short sentences with simple words.
- Use everyday language instead of medical language.
- Do everything you can to avoid medical terminology unless the client has high health literacy (e.g., physicians, nurses). Even still, this author tends to stick to lay terminology or use only medical words that are used in both fields of medicine. Never assume that a client that works in the medical field understands what you’re telling them. There are differences between human and veterinary diseases and treatments and, with the high degree of specialization in human medicine, they may not understand all facets of diabetes management if they’re a surgeon.
- Discharge instructions are important, but keep them relatively short. Give fewer instructions and consider using pictographs.
- Use concrete, explicit statements.
- Try to reduce client anxiety to a moderate level.
- Repetition may or may not help, but it can’t hurt.
- Recall can be improved by manipulating serial position of information and how you stress their importance.
Additional reading
- Bakker DA, Blais D, Reed E, et al. Descriptive study to compare patient recall of information: nurse-taught versus video supplement. Can Oncol Nurs J 1999;9:115-20.
- Bradshaw PW, Ley P, Kincey JA, et al. Recall of medical advice: Comprehensibility and specificity. Br J Soc Clin Psychol 1975;14:55-62.
- Delp C, Jones J. Communicating information to patients: the use of cartoon illustrations to improve comprehension of instructions. Acad Emerg Med 1996;3:264-70.
- Houts PS, Bachrach R, Witmer JT, et al. Using pictographs to enhance recall of spoken medical instructions. Patient Educ Couns 1998;35:83-8.
- Jansen J, Butow PN, van Weert JCM, et al. Does age really matter? Recall of information presented to newly referred patients with cancer. J Clin Oncol 2008;26:5450-7.
- Ley P. Primacy, rated importance and recall of medical information. J Health Soc Behav 1972;13:311-7.
- Ley P, Spelman MS. Communications in an outpatient setting. Br J Soc Clin Psychol 1965;4:114-6.
- McCann DP, Blossom HJ. The physician as a patient educator: From theory to practice. West J Med 1990;153:44-49.
- McCarthy DM, Waite KR, Curtis LM, et al. What did the doctor say? Health literacy and recall of medical instructions. Med Care 2012;50(4):277-82.
- McClement SE, Hack TF. Audio-taping the oncology treatment consultation: a literature review. Pat Educ Couns 1999;36:229-38.
- McGuire LC. Remembering what the doctor said: Organization and adults’ memory for medical information. Exp Aging Res 1996;22:403-428.
- Ong LM, de Haes JC, Hoos AM, et al. Doctor-patient communication: a review of the literature. Soc Sci Med 1995;40:903-18.
- Patwardhan M, Coeytaux RR, Deshmukh R, et al. What is the impact of physician communication and patient understanding in the management of headache? Neuropsychiatr Dis Treat 2007;3:893-7.
- Pavlik V, Brown AE, Nash S, et al. Association of patient recall, satisfaction, and adherence to content of an electronic health record (EHR)-generated after visit summary: A randomized clinical trial. J Am Board Fam Med 2014;27:209-218.
- Selic P, Svab I, Repolusk M, et al. What factors affect patients’ recall of general practitioners’ advice? BMC Family Practice 2001;12:141.
- van der Meulen N, Jansen J, van Dulmen S, et al. Interventions to improve recall of medical information in cancer patients: a systematic review of the literature. Psychooncol 2008;17:857-68.
- van Merriënboer JJG, Sweller J. Cognitive load theory in health professional education: design principles and strategies. Med Educ 2010;44:85-93.
- Werner A, Holderried F, Schäffeler N, et al. Communication training for advanced medical students improves information recall of medical laypersons in simulated informed consent talks – a randomized controlled trial. BMC Med Educ 2013;13:15.
About the author
In addition to his love of neurology and neurosurgery, Dr. Troxel is also interested in the use of technology to better care for patients and their owners and to improve efficiency in the veterinary clinic. |




