Current Diagnostic Approaches to Chronic Diarrhea (Part I)
Marion D. Haber, DVM, DACVIM
Massachusetts Veterinary Referral Hospital
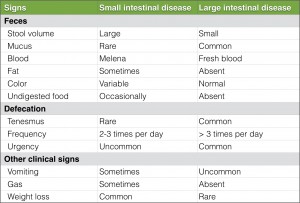
Diarrhea is described as an increase in fecal mass, specifically volume, frequency or fluidity, and it is an important clinical sign of intestinal disease. Diarrhea as a clinical sign can be found with both small and large intestinal disease. There are several differentiating factors (Table 1). Signs localizing to both the large and small intestine may be present in one clinical case. It is important to note, however, that small intestinal disease can be present without the actual presence of diarrhea.
Characterizing diarrhea
It may be helpful to employ a fecal scoring system (Fig. 1), such as the one provided by Purina, Inc., to help in further characterizing diarrhea. A fecal scoring system not only helps with characterization at the time of diagnosis, but it can also aid in judging response to treatment. It is also important to define the duration of diarrhea. Diarrhea that has been occurring for less than 7-14 days is considered acute, whereas diarrhea occurring greater than 21 days is considered chronic. Gathering this information along with a thorough history and physical examination helps in forming a plan to establish an appropriate diagnosis.
Diagnostic approaches to chronic diarrhea
Fecal examination is an essential tool in the diagnosis of diarrhea. The most common fecal test is fecal floatation to identify ova or cysts. Repeat testing of up to three separate fecal samples is recommended to diagnose intermittently shedding parasites. In cases of chronic diarrhea, prophylactic deworming should be considered even if fecal testing has been negative. Direct fecal examination evaluates for excess fungal or bacterial elements (e.g. Clostridium spp), but results can be misleading and need to be interpreted with other patient information. Some normal patients will have higher than normal spores or bacteria without diarrhea. Special stains for fat, starch, or muscle fibers can be applied to fecal smears to identify features of malabsorption. A fecal wet mount can be used to look for Campylobacter spp and trophozoites, such as those seen with Giardia spp. Rectal scraping for cytology should be examined for evidence of inflammation, as well as for evidence of fungal elements. Fecal culture should be pursued if inflammatory cells are noted on cytology or if significant hemorrhagic diarrhea and pyrexia are associated with diarrhea. A fecal culture, most commonly performed to check for Salmonella, Campylobacter jejuni, and Clostridium difficile, should be interpreted in light of other clinical signs. This diagnostic technique should not be used to aid in the diagnosis of small intestinal bacterial overgrowth. ELISA tests are commercially available for the detection of C. perfringens and C. difficile toxins, Giardia spp, Feline Panleukopenia Virus, and Cryptosporidium spp. Testing for these infections should be performed if indicated in those cases where exposure to these organisms appears likely (e.g., patients frequenting a boarding facility). PCR testing for Tritrichomonas spp in cats should be pursued in any cat with chronic large bowel diarrhea that is otherwise healthy. More information about this infection will be provided in Part II of this series next week. The fecal alpha1-proteinase inhibitor test is used to help in the diagnosis of protein losing enteropathy. It can be used to mark protein loss and is viewed as a more sensitive marker than serum albumin. This diagnostic test requires three fresh fecal samples, and it is important to note that gastrointestinal bleeding will cause this diagnostic test to be invalid.
Bloodwork
In cases of chronic unresponsive diarrhea where fecal testing is inconclusive, complete blood work including complete blood count, chemistry profile, and thyroid testing should be pursued to evaluate for other disease processes of the body. FeLV and FIV testing should be performed in cats as part of a complete evaluation. Radiographic imaging is important for identification of intestinal obstruction or displacement, masses, free gas, ileus, and serosal detail. Contrast imaging can also be helpful in the diagnosis of motility disorders, ulceration, and obstruction.
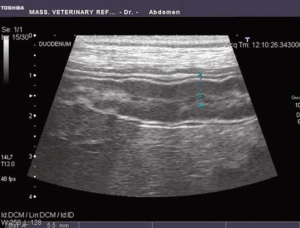
Fig. 2: Ultrasound image of thickened duodenum in a patient presenting with chronic small intestinal diarrhea
Ultrasound
Ultrasound is now more commonly used due to speed of evaluation and increased information obtained by this imaging modality. Ultrasound evaluation assesses intestinal wall thickness (Fig. 2) and layering. as well as for presence of masses, effusion, and other organ changes. It is important to note that a lack of intestinal wall change on ultrasound does not exclude the possibility of inflammatory bowel disease or lymphoma. Any data that is gathered must be interpreted in light of the patients presenting clinical signs and other test results.
Localization of Intestinal Disease
Evaluation of digestive function can be helpful in localization of intestinal disease. Trypsin-like immunoreactivity (TLI) testing measures trypsinogen, but also detects trypsin and some trypsin molecules bound to proteinase inhibitors. This test is used for evaluation of the adequacy of pancreatic function and is used for diagnosis of exocrine pancreatic insufficiency (EPI). Pancreatic lipase immunoreactivity (PLI) is alternatively suited for diagnosis of pancreatitis. This immunoassay measures pancreatic lipase and is highly specific for pancreatic function. There is a larger residual amount of pancreatic lipase remaining in the vascular space compared to trypsinogen so PLI testing is not used for the diagnosis of EPI. Intestinal function can in part be assessed using quantification of serum cobalamin (Vitamin B12) and folate. Vitamin B12 deficiency is a marker for distal small intestinal disease and is secondary either to the inability to absorb Vitamin B12 due to mucosal malabsorption or binding of Vitamin B12 by bacteria, such as may be seen with small intestinal bacterial overgrowth. Serum folate blood concentration evaluates for proximal small intestinal disease where deficiency is an indicator of malabsorption and excess is an indicator of bacterial overgrowth. Vitamin B12 deficiency usually worsens the signs of the GI disease that are already present. Rarely neurologic signs can be seen. Differentials for Vitamin B12 deficiency include severe, chronic small intestinal disease, pancreatic insufficiency, or hereditary causes. Breeds in which hereditary Vitamin B12 deficiency has been reported include Giant Schnauzer, Beagle, Border Collie, Australian Shepherd and Chinese Shar Pei. Vitamin B12 deficiency has also been reported in cats.
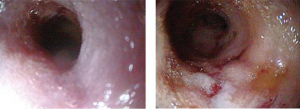
Fig. 3: Increased mucosal granularity and friability of the duodenum noted with endoscopic evaluation
Endoscopy or surgery
For definitive diagnosis of chronic diarrhea, biopsy may be necessary and it is important to decide between obtaining surgical or endoscopic biopsies. Endoscopy allows for gross examination, including mucosal granularity, friability (Fig. 3), levels of erythema, erosions and ulcers, retained food, and mass lesions. Endoscopy allows for collection of multiple tissue samples, although these samples do not penetrate all of the layers of the intestines. It can also aid with removal of foreign bodies and, at times, parasites may be visualized on examination. While there are many benefits to endoscopy, there are also limitations including the inability to obtain full thickness biopsies or to reach the jejunum and in smaller dogs and cats, the ileum. Ultrasound is very important in aiding to localize disease especially localizing what part of the intestine may be affected as well as what layers of the intestines.
Surgical biopsies are usually recommended for cases where endoscopic biopsies will likely not provide an accurate diagnosis for the cause of the diarrhea. Additional benefits to surgical biopsies include evaluation of other organs and the potential for corrective surgery. Specific disadvantages to surgery include surgical risk, dehiscence,and the need for a delay before starting steroids to avoid a delay in post-operative healing.
Once histopathology results are obtained via either surgical or endoscopic method, treatment is pursued. There are some rare cases where histopathology shows no abnormalities. In these cases differential diagnoses to be considered include small intestinal bacterial overgrowth, food sensitivity, toxin exposure, motility disorder, patchy mucosal disease or congenital disease.
Diagnosis of diarrhea can often be difficult, and due to client and patient considerations, a complete evaluation may not be possible. Trial with different treatments may be necessary.
Chronic diarrhea, Part II
Part II of this series will be posted next week. This will include a full discussion on treatment options for chronic diarrhea, as well as a more detailed update on two causes of chronic diarrhea.